You are here: vision-research.eu » Vision Research » The Young Researchers View » The Young Researcher's View: Kristina Irsch (Q1-2021)
The Research of Kristina Irsch
 |
Background
With a background in physics, I specialize in ophthalmic optics and instrument development. I received my PhD from Heidelberg University under the mentorship of Prof. Josef F. Bille. During my graduate studies I also worked at the Johns Hopkins Wilmer Eye Institute in Baltimore where I followed up with a postdoctoral research fellowship in ophthalmology under the supervision of Prof. David L. Guyton.
In 2010 I became an Assistant Professor of Ophthalmology at the Johns Hopkins University School of Medicine, merging my background in physics with endeavors in the field of ophthalmology to help bridge the gap between clinicians and engineers. My focus has been in the development and translation of diagnostic screening devices for remote detection of vision disorders in young children (e.g., Irsch K, et al. Opt Express 2014; Irsch K, et al. J Biomed Opt 2014). In 2014, I came to Paris to work at the Vision Institute / Quinze-Vingts National Eye Hospital on the development of high-resolution ocular imaging methods. In particular, I have been focused on developing an objective and quantitative assessment of human corneal transparency, in a project supported by a Horizon 2020 Marie Curie Reintegration Fellowship.
I have recently been named a Centre National de la Recherche Scientifique (CNRS) research scientist. My current scientific work is focused on solving problems inherent to ophthalmic imaging in patients, as well as on turning these problems, such as eye movements and light scattering, to potential advantage. The overall goal is to exploit the potential of the cornea and the eye to serve as a window into systemic processes within the body.
Scientific work
The eye has long been recognized as a window to visualize internal structures and study pathophysiological mechanisms. Remarkable developments in imaging technologies, including Optical Coherence Tomography (OCT) and more recently adaptive-optics retinal imaging, enabled for the first time the direct visualization and examination of the walls of blood vessels in vivo. However, many deeper cellular and sub-cellular ocular and retinal surctures still cannot yet be adequately visualized, especially in those with pathology.
Apart from patient motion, a major obstacle to ophthalmic imaging has been the imperfect transparency of intervening ocular media, notably the cornea and crystalline lens, in older individuals. Imperfect transparency is also the leading cause of blindness worldwide as a result of scattering of light worsening due to infections, other pathology, trauma, aging, or surgery. Unfortunately, no objective and quantitative clinical tool exists to assess such transparency, or its lack thereof.
The following paragraphs outline recent activities and preliminary progress towards the development of innovative tools to address and overcome these critical impediments in ophthalmic imaging.
Topic 1: Tackling the characterization of corneal transparency with tailored instrumentation
(a) Characterization of corneal transparency
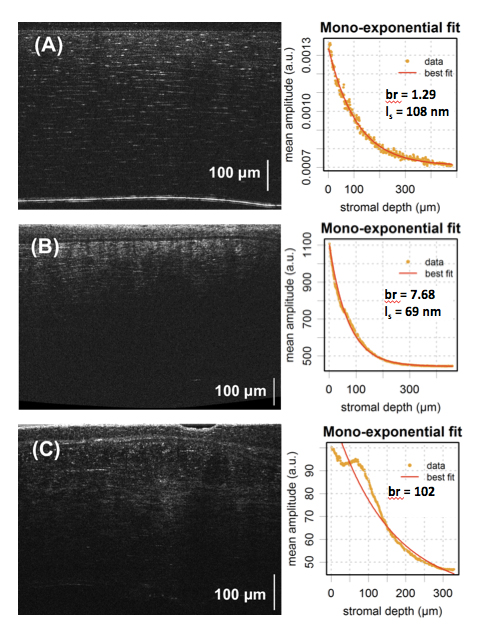
In collaboration with Prof. Karsten Plamann, from the Laboratory for Optics & Biosciences, École Polytechnique, we have been developing an optical data analysis-based approach to objective transparency assessment. Our method is based on a physical model of corneal transparency using stromal light scattering as objective indicator and was validated with ex vivo full-field OCT (Bocheux R, et al. PLoS One 2019). It enables the extraction of quantitative parameters, including the scattering mean-free path, a major indicator of scattering extent and thus of transparency of a medium (Fig. 1).
While ongoing work seeks to make full-field OCT suitable for in vivo examination (see below), our method may already be applied to current standard clinical depth-resolved imaging modalities, including spectral-domain (SD) OCT, and thereby enable objective and quantitative transparency assessment in the clinical setting. We are pursuing this clinical application in collaboration with Prof. Vincent Borderie’s anterior-segment service at the Quinze Vingts.
(b) Tailored instrumentation for cornea characterization
In collaboration with Prof. Claude Boccara’s group at the Langevin Institute, ongoing activities seek to make full-field (FF) OCT suitable for in vivo examination. While during Dr. Viacheslav Mazlin’s earlier doctoral work, we could demonstrate in vivo acquisition of en face images of diverse corneal layers, by integrating an ultrahigh-speed CMOS camera, air microscope objectives, and a near-infrared LED source (Mazlin V, et al. Biomed Opt Exp 2018), several challenges remain on the road to clinical translation.
One such challenge includes accounting for the living eye’s perpetual motion, which interferes with the acquisition of continuous volumes while limiting the reproducibility of quantitative measurements. A major source of such involuntary eye motion is from vascular pulsation and respiration manifesting itself in the axial direction.
In collaboration with Prof. Jin Kang’s group at the Johns Hopkins Whiting School of Engineering, we have been (Irsch K, et al. Proc of SPIE 2018) exploring axial-motion compensation techniques with OCT.
One possibility to account for involuntary axial eye motion with FF-OCT is via the integration of a distance sensor, based on SD-OCT, to locate the target (corneal) surface from individual A scans, and then sending a feedback control signal to a motor that dynamically controls the focus via re-positioning of the reference arm. We developed such a combined (common-path) FF-OCT and SD-OCT in vivo microscope and demonstrated real-time and consistent FF-OCT performance through axial eye tracking and simultaneous defocus correction (Mazlin V, et al. Nat Commun 2020).
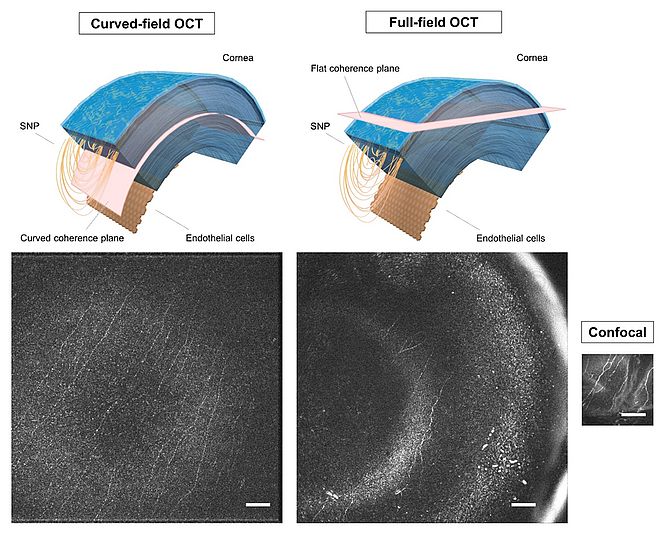
Within the scope of this collaboration, we have recently re-designed the in vivo FF-OCT microscope, by replacing the flat mirror in the reference arm with an optical lens acting as a curved reference mirror. Note that if the sample is curved, such as the cornea that exhibits natural curvature, the previously employed flat reference mirror optically sections through several (corneal) layers at once, keeping the FF-OCT’s field-of-view of individual fine layers limited. The use of a curved reference mirror, on the other hand, in what we termed “curved-field (CF) OCT” allows to curve the coherence gate and obtain optical sections of arbitrary curvature (Mazlin V, et al. Optica 2020). Applied to the in vivo human cornea, we demonstrated that CF-OCT is capable of capturing large-field views of individual layers, such as the fine sub-basal nerve plexus (SNP; Fig. 2) and endothelium, well beyond what is currently possible with state-of-the-art clinical approaches.
Topic 2: Establishing the foundation for compensation of corneal transparency imperfections and loss
To further enhance FF-OCT technology, we are also exploring light manipulation techniques, specifically the implementation of an array-illumination and backscattering-matrix approach (Badon A, et al. Sci Adv 2020). Beyond enabling deeper penetration into the corneal tissue and the characterization of other ocular media, this approach has implications for imaging through ocular media opacities (e.g., imaging the retina when there is loss of ocular media transparency, such as imaging through cataract opacities). This collaboration with Dr. Alexandre Aubry, at the Langevin Institute started within the scope of Amaury Badon’s, and then Victor Barolle’s PhD theses, who obtained the first proof-of-concept demonstration of imaging through a cloudy (edematous) cornea ex vivo (Fig. 3).
Topic 3: Using light scattering for high-resolution retinal imaging
A further interesting aspect of our recent research suggests that deliberate use of scattering media to illuminate the retina could provide new imaging opportunities. With support of the National Institutes of Health, in collaboration with Prof. Rafael Piestun from the University of Colorado Boulder, we are exploring ambitious approaches for imaging the ocular fundus.

Kristina Irsch, PhD
Research Scientist – CRCN, CNRS
Vision Institute, CNRS UMR 7210
17, rue Moreau
75012 Paris
France
E-mail: kristina.irsch[at]inserm.fr